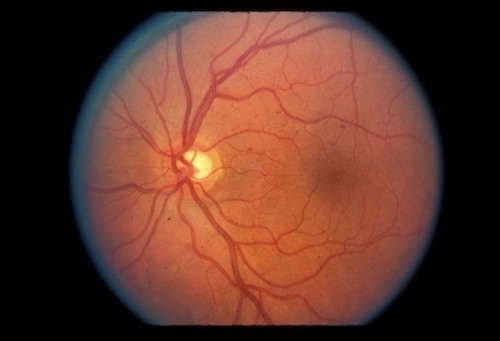
What is Diabetic Retinopathy?
Diabetes is a systemic and metabolic disease with high blood sugar levels. Diabetes that impacts the entire body particularly affects our organs, including small vessels. The eyes are one of them. The most important effect of diabetes in the eye is badly affects the nutrition of the small nerve layers. As a result, bleeding, deposits, fluid collection, edema occur in the retina layer. This called diabetic retinopathy.
What are the symptoms of diabetic retinopathy?
Retinal edema occurs in the center of vision that we call macula and gradually leads to decreased vision. In some cases, there are no symptoms without fluid collection and there is insidious intraocular bleeding which causes loss of vision.
How is diabetic retinopathy diagnosed?
Diabetes patients should be examined immediately after diagnosis. In the ophthalmologic examination, diabetic retinopathy canbe diagnosed. To evaluate the degree of diabetic retinopathy and treatment options after diagnosis, eye tomography (OCT) and eye angiography (FFA) should be performed.
What are the options of diabetic retinopathy treatment?
The most important step in the treatment is control to prevent high blood pressure, blood cholesterol and blood sugar. If diabetic retinopathy develops, argon laser photocoagulation is performed according to the degree of eye angiography and tomography. If there is edema in the macula, intraocular needle therapy is on the agenda. Usually single-session laser or needle therapy is not enough. In advanced cases, intraocular bleedings and tapes formed by the surgery called vitrectomy can be cleaned.
In what range should eye control be done in diabetes?
When diabetes is diagnosed, the first eye examination should be performed. Then, if there is no problem, the examination should be done at least once a year. Following the start of diabetic retinopathy, the duration of follow-up can be reduced by 1-6 months.
